10 reasons your blood sugar might be out of range (that have nothing to do with what you ate)
We're so quick to blame food when our blood sugar is off. Makes sense when "diet and exercise" is basically the only message most of us ever hear. But diabetes is soooo much more complex than that. Ever eaten the exact same thing at the exact same time two days in a row with completely different outcomes? That’s NORMAL (and yeah, can be annoying)
Understanding the many things that can affect blood sugar isn't just useful information; it can also help you approach your body with more curiosity and a lot more compassion. While this certainly isn’t an exhaustive list, these are conversations that come up most often with the people I work with.
Stress
I’m starting here because, in my opinion, this is the most frustrating one on the list and it’s going to come up again later. When we're stressed, our bodies release cortisol, which makes our cells less able to absorb sugar from the blood, also known as insulin resistance.
There's actually a good evolutionary reason for this. For early humans, danger was often fast and physical: a predator, a threat, something to fight or run from. Their bodies would flood with cortisol and glucose to give them energy to run, fight, hide, and survive. Once the danger passed, cortisol was flushed out, bodies relaxed, and blood sugar came back down.
The problem is that modern stress doesn't work that way but our bodies still do. In today’s world, stress is often chronic. A stressful job, money, reproductive rights being slashed, a fascist government (yeah, you bet I’m getting political- health IS political). We have less opportunities to RUN to safety and then calm down, also known as completing our stress cycle. There is ALWAYS something to stress about, and it’s unlikely many of these stressors will end soon (making stress “chronic.”)
It might be most useful to think about the ways you can best complete your stress cycle, signaling to the body that you are as safe as possible. How can you help your nervous system find it’s way back to calm? This might look like movement, creative expression, or connection with people who feel safe to you. For a deeper dive into this concept, I love the book Burnout by Amelia and Emily Nagoski.
2. Sleep
Poor sleep, whether in quality or quantity, can make it harder to keep your blood sugar in range. Research suggests that getting fewer than 7 hours a night is associated with increased insulin resistance, likely connected to elevated inflammation markers in the body (like CRP and serum ammyloid-a) (1).
While we don’t yet know exactly why this is, there is still a strong correlation and something to consider when thinking about your diabetes care. If your blood sugar has been harder to manage lately, it's worth asking: how has my sleep been?
3. Your Menstrual Cycle
If you menstruate and track your cycle, you may have already noticed this: blood sugar can feel almost effortless to manage at some points in your cycle, and much harder at others.
During the luteal phase (the second half of your cycle, after ovulation and before your period) progesterone is running the show. One of progesterone's many jobs is basically to "hold on to things”: your uterine lining, a potentially fertilized egg, slowing digestion (hello, bloating, constipation, and reflux), and yes, sugar in the blood. Progesterone creates more insulin resistance, which can make your numbers harder to manage during this window.
Evolutionarily, this makes some sense: the body wants to ensure there's plenty of fuel available in case of pregnancy. But if you have diabetes, have a period, and aren’t pregnant? Kind of annoying.
Some things that might help? If you take insulin, you may need slightly more insulin during this time. Prioritizing fiber, protein, and quality sleep can also help and as always, being gentle with yourself goes a long way (andddd what do you know, we’re back to #1: stress impacts blood sugar)
4. Insulin that’s gone bad
If you use insulin and you've noticed your blood sugars are suddenly harder to bring down but you can't figure out why, it might be worth checking your insulin. Most insulins are effective for about 28 days once opened (or oxygen is introduce into the vial via a syringe) or removed from the fridge. After that, potency drops.
Effectiveness of your insulin can also be decreased by heat. For example, a vial left in a hot car won't survive.
Depending on how much insulin you use, you may find yourself throwing out a bit at the end of the month.
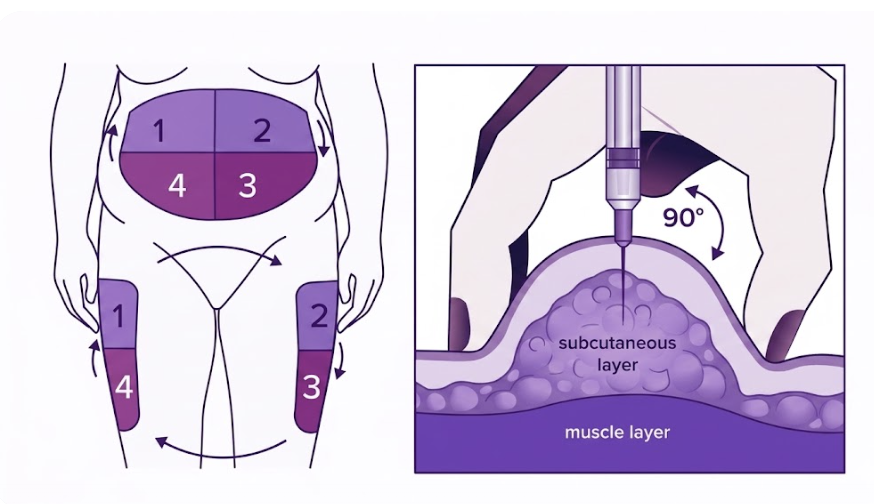
5. Injection and infusion sites
If you use insulin, the location and condition of your injection and insulin pump sites matters.
Over time, repeatedly using the same spots can cause scar tissue to build up, which make insulin absorption slower and more unpredictable. Rotating your sites regularly helps to prevent a build up of scar tissue.
It's also worth knowing that different parts of the body absorb insulin at different speeds, largely based on blood flow. In general: the abdomen absorbs fastest, followed by the arms, then the legs and butt (2). You can actually use this to your advantage by using faster-absorbing spots for mealtime or correction insulin, slower-absorbing spots for long-acting insulin.
6. Altitude
This one surprises a lot of people. Being at higher altitude can actually lower blood sugar (3). The air is thinner, so your body has to work harder to deliver oxygen to your muscles, which uses energy similarly to exercise, even when you're resting. Body works harder→ sugar in the blood is moved into the muscles for energy→ blood sugar is lowered.
If you use insulin or a medication that carries a risk of low blood sugar (like a sulfonylurea or insulin), it's worth planning ahead when traveling to higher elevations like adjusting your dose and keeping extra snacks on hand.
BUT, because bodies are, of course, complex, the initial change in altitude can sometimes briefly raise blood sugar, since any sudden shift is a mild stressor on the body.
Your body will usually acclimate after a few days to weeks.
7. Illness or Infection
Being sick is stressful on the body (surprise surprise), and your body responds accordingly: releasing cortisol and epinephrine to activate your immune system. Both hormones increase insulin resistance, which is why blood sugars often run higher when you're under the weather, even if you're not eating or moving as much.
Fun fact, there is a good reason for this connection: Active immune cells (cells that are fighting off invaders) are VERY hungry and primarily use sugar/glucose for energy since it’s the fastest form of energy. Having more sugar in the blood may be super helpful so that active immune cells have an abundance of nutrition (4).
This is normal, and it's not your fault. Give yourself extra grace when you're sick and take time to rest and recover. It can also be helpful to build yourself a sick day plan that includes how you’ll stay hydrated and safe during sickness.
8. High blood sugar itself
I know… this one feels deeply unfair. But sustained high blood sugar can actually make it harder to bring blood sugar down. You might have noticed times when your numbers feel "stuck" even when you've done everything right. That’s caused by glucotoxicity (5).
When blood sugar stays elevated for a prolonged period, it can limit the body's ability to produce insulin, cause increased inflammation, and slow down the process of converting sugar into energy. High blood sugar causes more high blood sugar. It's a frustrating cycle.
The approach here is typically patience and gentleness: staying hydrated, resting, using your tools as directed, and gentle movement if your blood sugar isn't too high. For some people, a short course of additional insulin can help break the cycle; your doctor can help you figure out if that's appropriate for you.
9. Aging
Insulin resistance tends to increase naturally as we age. Our bodies' ability to process sugar slows down over time. This is largely genetic or epigenetic, meaning it's not something you caused or could have prevented.
For some people, this shift is barely noticeable and their bodies compensate. For others, it may mean a new diagnosis or a need for additional medication. Either way, it's a normal part of how bodies change, not a reflection of how well you've been taking care of yourself.
10. Temperature and weather
Yes, really, the weather can affect your blood sugar. In general, hot weather tends to lower it (blood vessels dilate to help cool you down, increasing blood flow and insulin absorption), while cold weather can act as a stressor and increase insulin resistance, often leading to higher blood sugar.
That said, it's complicated (as with EVERYTHING!). For people who can't easily go outside in extreme heat, warmer months might mean less movement. And when hot weather causes dehydration, it can raise blood sugar. Bodies are frustratingly (and wonderfully) complex.
If any of this resonates or if you've been hard on yourself about numbers that were never really about your “diet,” I hope this gives you a little more room to breathe. Managing diabetes is genuinely complicated, and you deserve support that acknowledges that.
References
Singh T, Ahmed TH, Mohamed N, et al. Does Insufficient Sleep Increase the Risk of Developing Insulin Resistance: A Systematic Review. Cureus. 2022;14(3):e23501. Published 2022 Mar 26. doi:10.7759/cureus.23501
Gradel AKJ, Porsgaard T, Lykkesfeldt J, et al. Factors Affecting the Absorption of Subcutaneously Administered Insulin: Effect on Variability. Journal of Diabetes Research. 2018;2018(1205121). doi:https://doi.org/10.1155/2018/1205121
de Mol P, de Vries ST, de Koning EJP, Gans ROB, Bilo HJG, Tack CJ. Physical Activity at Altitude: Challenges for People With Diabetes. Diabetes Care. 2014;37(8):2404-2413. doi:https://doi.org/10.2337/dc13-2302
Hosomi K, Kunisawa J. Diversity of energy metabolism in immune responses regulated by micro-organisms and dietary nutrition. Int Immunol. 2020;32(7):447-454. doi:10.1093/intimm/dxaa020
Glucotoxicity - an overview | ScienceDirect Topics. www.sciencedirect.com. https://www.sciencedirect.com/topics/medicine-and-dentistry/glucotoxicity